The healthcare industry relies heavily on accurate and efficient record-keeping. One of the most crucial components of this process is the Icu Progress Note Template. This standardized document provides a concise and detailed record of a patient’s condition and treatment during their stay in the intensive care unit (ICU). A well-structured Icu Progress Note Template is vital for seamless communication between healthcare providers, ensuring continuity of care and facilitating informed decision-making. This guide will delve into the key elements of an effective Icu Progress Note Template, covering its purpose, structure, and best practices. Understanding and utilizing this template effectively can significantly improve patient outcomes and streamline workflows within the hospital setting. Icu Progress Note Template is more than just a form; it’s a tool for patient safety and operational efficiency.
The primary function of an Icu Progress Note Template is to capture essential information about a patient’s condition and response to treatment. It’s a dynamic document, frequently updated throughout a patient’s stay, reflecting their evolving needs and the interventions administered. It’s designed to be readily accessible to healthcare professionals, allowing them to quickly assess a patient’s status and initiate appropriate care. Without a standardized template, communication could be fragmented and potentially lead to errors in diagnosis and treatment. The template’s consistent format ensures that all relevant information is captured, regardless of the specific circumstances. It’s a cornerstone of quality patient care.
Understanding the Purpose of an Icu Progress Note Template
Before diving into the specifics of the template, it’s important to grasp why it’s so critical. The template’s core purpose is to provide a clear and objective record of a patient’s clinical status. This allows clinicians to:
- Track Patient Progress: The template facilitates continuous monitoring of a patient’s condition, allowing for early detection of deterioration.
- Document Treatment: It meticulously records all interventions, medications, and responses to treatment, providing a complete history of the patient’s care.
- Facilitate Communication: The standardized format ensures that all relevant information is readily available to other healthcare providers involved in the patient’s care.
- Support Decision-Making: Detailed records provide a strong foundation for informed clinical decisions, including adjustments to treatment plans.
- Compliance: Many healthcare facilities require Icu Progress Note Templates for regulatory compliance, ensuring accurate and complete documentation.
The template’s structure is carefully designed to minimize ambiguity and maximize clarity. It’s not simply a list of symptoms; it’s a narrative that conveys the patient’s experience.
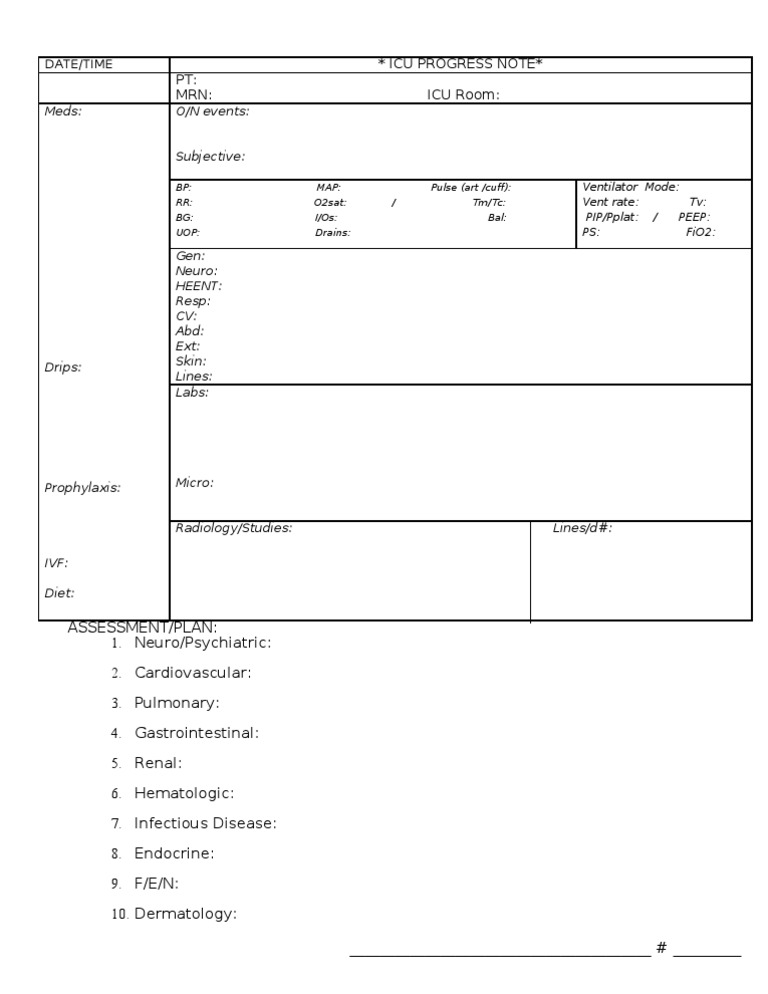
The Core Sections of an Icu Progress Note Template
Let’s examine the key sections that comprise a typical Icu Progress Note Template. Each section is designed to gather specific information relevant to the patient’s current state.
Section 1: Patient Demographics
This section includes essential patient information, such as:
- Patient Name: Full name of the patient.
- Medical Record Number (MRN): Unique identifier for the patient.
- Date of Birth: Patient’s date of birth.
- Gender: Patient’s gender.
- Contact Information: Phone number and emergency contact details.
Section 2: Initial Assessment
This section provides a preliminary overview of the patient’s condition upon admission. It typically includes:
- Chief Complaint: The patient’s primary reason for admission.
- History of Present Illness (HPI): A detailed description of the patient’s current symptoms and their onset.
- Vital Signs: Temperature, heart rate, blood pressure, respiratory rate, and oxygen saturation.
- Physical Examination Findings: Observations made during the physical examination, including any abnormalities.
Section 3: Ongoing Assessment & Treatment
This is the heart of the template, detailing the patient’s current condition and the interventions administered. It includes:
- Current Condition: A concise summary of the patient’s current state, reflecting their response to treatment.
- Medications: A list of all medications the patient is currently taking, including dosage and frequency.
- Vital Signs: Updated vital signs, noting any changes.
- Interventions: A detailed record of all interventions performed, including the type of intervention, the time of administration, and the healthcare provider involved. This section is crucial for tracking treatment effectiveness.
- Diagnostic Tests: Results of any diagnostic tests performed (e.g., blood tests, imaging studies).
Section 4: Response to Treatment
This section focuses on how the patient is responding to treatment. It’s a critical area for monitoring treatment effectiveness.
- Response to Medications: Assessment of the patient’s response to medications, noting any side effects or adverse reactions.
- Response to Therapy: Evaluation of the patient’s response to any therapeutic interventions, such as physical therapy or rehabilitation.
- Patient’s Comfort Level: Assessment of the patient’s comfort level, expressed through verbal or non-verbal cues.
Section 5: Additional Notes & Observations
This section allows for any additional relevant information to be recorded.
- Relevant History: Any pertinent medical history, allergies, or previous medical conditions.
- Social History: Information about the patient’s social history, including substance use and support systems.
- Family History: Relevant family history.
- Observations: Any other observations that may be relevant to the patient’s care.
The Importance of Standardization and Consistency
Maintaining a consistent and standardized Icu Progress Note Template is paramount for ensuring data quality and facilitating efficient communication. Variations in formatting, terminology, and content can lead to inconsistencies and errors. Adherence to a pre-defined template ensures that all relevant information is captured in a consistent manner. Training healthcare professionals on proper template usage is essential for maintaining accuracy and completeness.
Conclusion: Leveraging the Icu Progress Note Template for Optimal Patient Care
The Icu Progress Note Template is an indispensable tool for healthcare professionals. Its structured format, comprehensive coverage, and emphasis on clear communication contribute significantly to improved patient outcomes and streamlined workflows. By consistently utilizing this template, healthcare providers can ensure accurate and timely documentation, facilitating informed decision-making and ultimately enhancing the quality of patient care. Investing in proper training and adherence to the template’s guidelines is a vital investment in the overall efficiency and effectiveness of the healthcare system. Ultimately, a well-utilized Icu Progress Note Template empowers clinicians to provide the best possible care to their patients.