The healthcare industry is increasingly reliant on electronic medical records (EMRs) and digital documentation. One of the most crucial components of this digital transformation is the Soap Note Template Word, a standardized format for capturing patient information and clinical notes. This article will delve into the purpose, benefits, creation, and best practices for utilizing a robust Soap Note Template Word to streamline workflows, improve patient care, and enhance data analysis. Understanding how to effectively implement and utilize this template is vital for healthcare professionals seeking to optimize their practice. The core function of a well-structured Soap Note Template Word is to provide a clear, concise, and easily accessible record of a patient’s encounter, facilitating seamless communication between providers and ensuring continuity of care. It’s more than just a document; it’s a vital tool for quality improvement and operational efficiency.
What is a Soap Note Template Word?
A Soap Note Template Word is a standardized, digital format designed for capturing patient information during clinical encounters. It’s a structured document that guides clinicians in documenting key details, ensuring consistency and facilitating efficient data retrieval. Unlike free-form handwritten notes, a Soap Note Template Word enforces a specific structure, promoting clarity and reducing the risk of errors. It’s a digital representation of the conversation, capturing the essence of the patient’s presentation, diagnosis, treatment plan, and progress. The template’s core elements typically include sections for demographics, chief complaint, history of present illness, physical examination findings, assessment, plan, and follow-up instructions. The goal is to create a readily accessible and easily searchable record of the patient’s care.
The Benefits of Using a Soap Note Template Word
Implementing a standardized Soap Note Template Word offers a multitude of benefits for healthcare providers and organizations. Firstly, it significantly improves data accuracy and completeness. By adhering to a consistent format, errors related to transcription or note-taking are minimized. Secondly, it streamlines workflows, reducing the time spent on documentation. Instead of manually transcribing notes, clinicians can quickly access the relevant information within the template. This leads to increased efficiency and reduced administrative burden. Thirdly, it enhances communication between providers. The standardized format facilitates seamless information exchange, ensuring that all relevant details are captured and shared effectively. Finally, it supports better patient care through improved documentation and continuity of care. A complete and accurate record allows for more informed decision-making and facilitates effective treatment planning.
Key Sections of a Standardized Soap Note Template Word
Let’s examine some of the essential sections commonly found within a Soap Note Template Word. Each section plays a critical role in capturing the complete picture of a patient’s encounter.
1. Patient Demographics
This section gathers essential information about the patient, including:
- Patient Name: Full name, including any nicknames.
- Date of Birth: Crucial for accurate record-keeping.
- Medical Record Number (MRN): A unique identifier for the patient.
- Contact Information: Phone number, address, and emergency contact details.
- Insurance Information: Policy number and group name.
2. Chief Complaint
This section clearly states the patient’s primary reason for seeking medical attention. It’s a concise and easily understandable description of the patient’s main concern.
- Example: “Patient presents with chest pain and shortness of breath.”
3. History of Present Illness (HPI)
This section provides a detailed account of the patient’s current condition, including:
- Onset: When did the symptoms begin?
- Location: Where is the pain or discomfort located?
- Character: What does the pain feel like (e.g., sharp, dull, aching)?
- Radiation: Does the pain radiate to other areas?
- Severity: How severe is the pain (e.g., on a scale of 1-10)?
- Timing: How long does the symptom last?
- Aggravating and Relieving Factors: What makes the symptoms worse or better?
4. Past Medical History (PMH)
This section outlines the patient’s previous medical conditions, surgeries, hospitalizations, and allergies.
- Chronic Conditions: Diabetes, hypertension, asthma, etc.
- Past Surgeries: List of previous surgeries, including dates and procedures.
- Allergies: Medications, food, environmental, and latex allergies.
- Immunizations: Vaccination history.
5. Medications
This section details all medications the patient is currently taking, including dosage, frequency, and route of administration.
- Prescription Medications: Name, dosage, frequency, and indication.
- Over-the-Counter Medications: List of OTC medications and dosages.
- Supplements: List of supplements and dosages.
6. Social History
This section covers the patient’s lifestyle factors, including:
- Smoking Status: Current smoker, former smoker, never smoked.
- Alcohol Consumption: Frequency and amount.
- Drug Use: History of illicit drug use.
- Occupation: Job and potential occupational hazards.
- Living Situation: Living alone, with family, etc.
7. Physical Examination Findings
This section summarizes the results of the physical examination performed during the encounter.
- Vital Signs: Temperature, blood pressure, heart rate, respiratory rate.
- General Appearance: Overall impression of the patient’s condition.
- HEENT (Head, Eyes, Ears, Nose, Throat): Examination of these areas.
- Cardiovascular: Auscultation of heart sounds.
- Respiratory: Auscultation of lung sounds.
- Abdomen: Palpation and assessment of abdominal organs.
- Neurological: Examination of the neurological system.
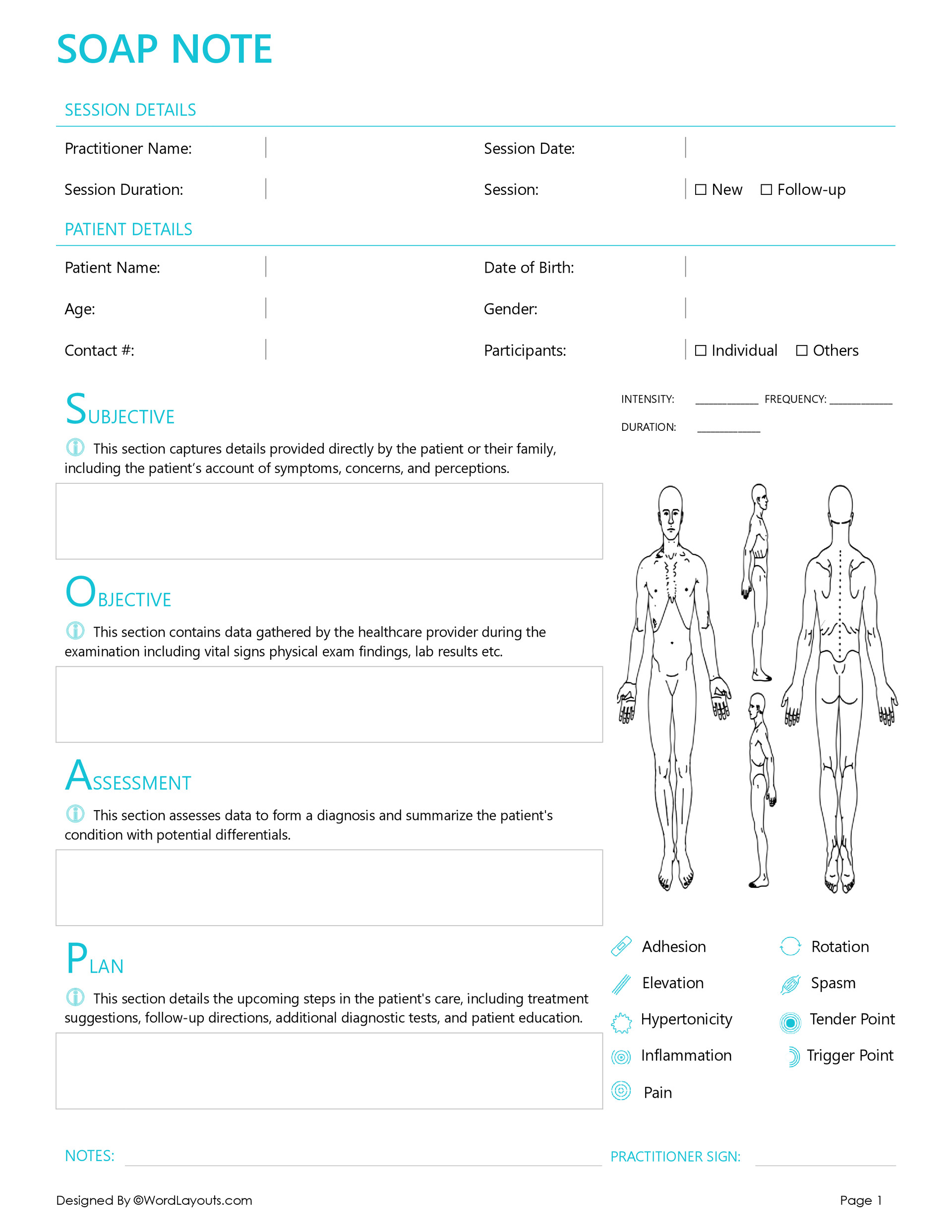
8. Assessment
This section provides the provider’s interpretation of the patient’s condition, including a diagnosis (if applicable) and differential diagnoses.
- Diagnosis: The primary diagnosis.
- Differential Diagnoses: Other possible diagnoses to consider.
9. Plan
This section outlines the proposed treatment plan, including:
- Medications: Prescribed medications, dosages, and instructions.
- Therapies: Physical therapy, occupational therapy, etc.
- Lifestyle Modifications: Recommendations for diet, exercise, and smoking cessation.
- Follow-up Instructions: When and how to schedule follow-up appointments.
10. Progress Notes
This section is a brief summary of the patient’s progress during the encounter. It’s a record of what was observed and any changes made to the plan.
The Importance of Standardization
The consistent use of a Soap Note Template Word is paramount for several reasons. It reduces variability in documentation, improves communication among providers, and facilitates data analysis. By standardizing the format, healthcare organizations can gain a more comprehensive understanding of patient care and identify areas for improvement. Furthermore, the use of templates allows for automated data capture, reducing the risk of errors and improving efficiency. Investing in a well-designed and implemented Soap Note Template Word is a strategic investment in quality patient care and operational effectiveness.
Beyond the Basics: Advanced Features and Considerations
While the core elements of a Soap Note Template Word remain consistent, there are increasingly sophisticated features being incorporated. Many platforms now offer features like:
- Image Capture: Ability to capture images of patient charts, medications, and other relevant documents.
- Voice Recognition: Automated transcription of notes.
- Integration with EMR Systems: Seamless integration with existing EMR systems for data exchange.
- Mobile Accessibility: Access to the template on mobile devices for clinicians in the field.
- Customization: The ability to tailor the template to specific clinical workflows and organizational needs.
It’s crucial to select a template that aligns with your organization’s specific requirements and workflows. Proper training and implementation are also essential for maximizing the benefits of a Soap Note Template Word. Regularly reviewing and updating the template ensures its continued relevance and effectiveness.
Conclusion
The Soap Note Template Word represents a fundamental shift in healthcare documentation, moving away from unstructured notes towards a structured, standardized approach. Its benefits – improved data accuracy, streamlined workflows, enhanced communication, and better patient care – are undeniable. By embracing this technology and consistently utilizing a well-designed Soap Note Template Word, healthcare providers can significantly improve the quality of care they deliver and contribute to a more efficient and patient-centered healthcare system. The continued evolution of this technology promises even greater improvements in the future, solidifying its position as an indispensable tool in modern healthcare.